Sexual Health Needs Assessment
This Needs Assessment describes the sexual health needs of residents of the London borough of Richmond upon Thames. It draws on evidence gathered through epidemiological analysis and has informed the development of the Sexual Health Strategy with a focus of prevention.
This document is also available in PDF format: LBRuT Sexual Health Needs Assessment 2018
1 Executive Summary
Unplanned Pregnancy
• Significantly lower under 18 conceptions compared with England and London
– a consistent trend over the last decade.
• Over 80% of teenage conceptions end in abortion, indicating a need for better education and access to contraception.
• Over two thirds (70.8%) of women use user dependent methods of contraception (UDM), this is higher than England (62%). Lower percentage of women using LARC compared to England.
• All age abortions rate similar to England.
Sexually Transmitted Infections
• STI rate similar to England.
• Genital warts rate is higher than England.
• Young people are the largest group diagnosed with new STIs.
• Over a fifth (22%) of 15-year-olds in Richmond have 3 or more risky behaviours, including smoking, drinking, cannabis, other drugs, diet and physical health, the highest in London.
• 10% of new STIs were diagnosed in Richmond residents aged between 45 and 65 years of age.
• Lesbian, gay, bisexual, transgender, questioning and intersex (LGBTQI) and black people experience a disproportionately high rate of STIs.
• Black population have an STI rate three and a half times that in the white population
HIV
• High prevalence area for human immunodeficiency virus (HIV).
• Between 2014 and 2016, over a third (35.3%) of people diagnosed with HIV were diagnosed late.
• The lifetime cost for treating one HIV infection in the UK is estimated to be almost £380,000, based on a median life expectancy of 71.5 years for men who have sex with men (MSM) diagnosed at the age of 30.
• Estimates suggest approximately 45 people are unaware they have HIV.
2 Introduction
Improving sexual health is a public health priority. Sexual health affects the population across the life course. Poor sexual health can have not only physical but mental health implications. STIs and unintended pregnancies can have long-lasting and costly impacts on both individuals and wider society. However, they can be reduced through safer sex practices such as the use of condoms and regular testing. Sexual health services currently focus on treatment for sexual health transmitted infections, HIV and
unplanned pregnancies as well as prevention. Evidence shows that a focus on prevention can improve sexual health and deliver savings to sexual health commissioners and the wider system.
2.1. Aim
This Needs Assessment report sets out the current and future challenges that maintaining good sexual health presents to people, their carers, friends and families, the local authority and the NHS in Richmond.
It seeks to identify key messages to guide the development of good quality, accessible sexual health services with an increased focus on prevention for the population of Richmond.
2.2. Audience
This Needs Assessment report is intended to inform the policies, strategies, development and commissioning plans, and practice in local organisations including council teams, NHS organisations such as the Clinical Commissioning Group (CCG) and NHS Trusts, and other organisations, such as the voluntary sector and representatives of the public and patients.
3 Background
The resident population in Richmond is 194,730. Overall the health of the population is better than the London and England average.
Sexual health is defined by WHO as “… a state of physical, mental and social wellbeing in relation to sexuality. It requires a positive and respectful approach to sexuality and sexual relationships, as well as the possibility of having pleasurable and safe sexual experiences, free of coercion, discrimination and violence” (WHO, 2006).
Sexual health is a whole population and life course issue; in early childhood children begin developing their sense of identity and relationships with those around them, and during adolescence young people begin to develop their independence and form sexual relationships. By adulthood most of the population are sexually active and require support, such as good contraceptive services, information and treatment services, to maintain good sexual health.
Poor sexual health can result in substantial costs to individual and society across health, housing, education and social care. Learning from the former national Teenage Pregnancy Strategy showed that the substantial reduction in teenage conceptions was delivered using a preventive approach.
Department of Health (DoH)/PHE (Public Health England) and partners have published several documents to support sexual health commissioning and prevention:
- A Framework for Sexual Health Improvement (2013)
- Making it work: a guide to whole system commissioning for sexual health,
reproductive health and HIV (2015). - Good progress but more to do: teenage pregnancy and young parents (2016).
- Improving the health and wellbeing of lesbian and bisexual women and other women who have sex with women (2018)
There are 3 sexual health indicators in the Public Health Outcomes Framework:
- Chlamydia detection rate (15 to 24-year olds)
- people presenting with HIV at a late stage of infection
- under 18 conceptions
The previous needs assessment was undertaken in 2014 using data relating to 2012, and, where possible, the current data (2016) is compared to it. Overall, sexual health outcomes in Richmond are similar to the England average. Since 2012, sexual health has improved with a reduction in the rate of STIs and teenage conceptions.
4 Local Picture
4.1 Unplanned Pregnancies
4.1.1 Teenage Conceptions
Teenage parents and their children experience poorer health, educational and economic outcomes and inequality (PHE, 2018). There is a strong relationship between teenage conceptions and deprivation; rates of teenage pregnancy and STIs are higher in deprived areas and some minority groups are disproportionately affected (Tanton et. al., 2015). Richmond upon Thames as a geographical area is in the least deprived decile (IMD 2015, PHE, 2018) and has a relatively low teenage conception rate.
In 2016, there were 32 conceptions in under 18-year-old women, which is a rate of 10.4 per 1,000 population and lower than the England (18.8) and London (17.1) rate. The estimated maternity rate in women under 18 is 1.9 per 1,000. This is a significant decrease from 2012 when there 53 conceptions in women under 18 and the rate was 19.9 in Richmond, lower than England (27.7) and London (25.9) (ONS, 2018). However, although there was a decrease in 2013 there has not been a consistent decrease in Richmond since 2012; the rate was 11.7 in 2013, 12.6 in 2014 and 12.9 in 2015.
Figure 1: Rates per 1000 population of conceptions in women aged under 18 by year in Richmond upon Thames compared to rates in areas of London PHE Centre (PHEC) and England: 2012-2016
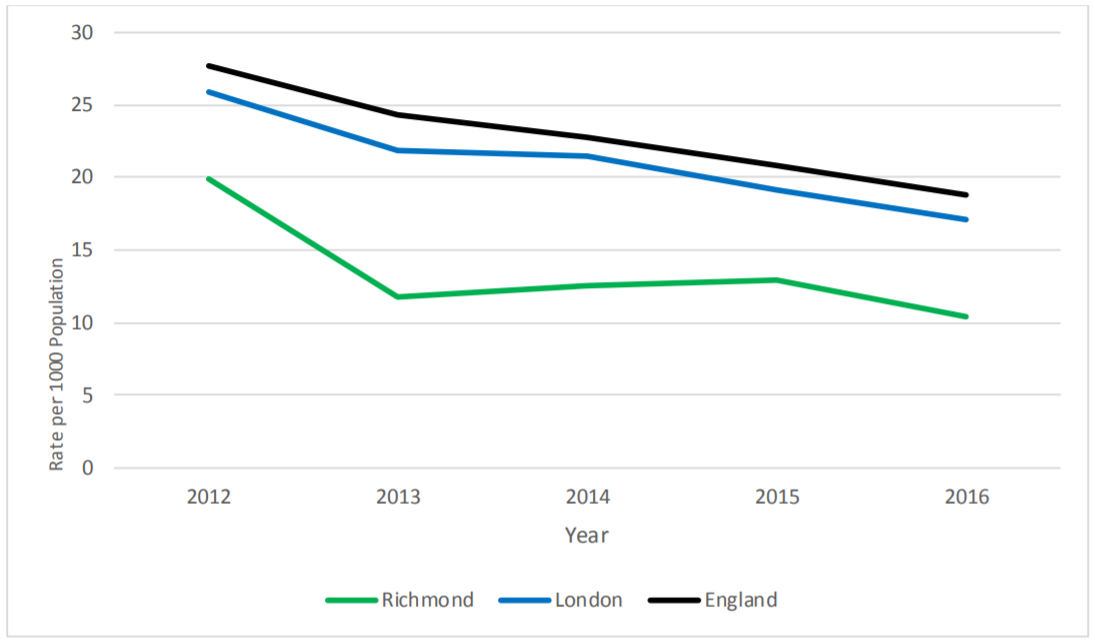
Source: Data from ONS. Rates based on the 2011 ONS population estimates.
4.1.2 Abortion
Termination of pregnancy (abortion) rates are used as a proxy measure for unplanned pregnancies. These pregnancies result from the absence of, incorrect or inconsistent use of contraception.
In 2016, 18.6% of total conceptions (547 abortions) in Richmond ended in abortion which was lower than England (21.8%) and London (25.4%). The largest number of abortions occurred in the 35+ age group (144), which is almost six times the number in under 18 age group (24) and three times the 18-19 age group (47) (ONS, 2018).
Almost 40% of all abortions (213 abortions) were repeat abortions, which consists of 42% of abortions in over 25s (62 abortions) and 33% in under 25 (151) (ONS, 2018). The percentage of repeat abortions (39%) is similar to London (41.9%) and England (38.4%).
However, at 81.3% the percentage of teenage conceptions ending in abortion, is significantly higher than England (51.8%) and London (63.7%). This reflects the inverse relationship between teenage conceptions ending in abortion and deprivation (Ellis, 2004).
4.1.3 Contraception
The main cause of unintended pregnancies is incorrect and inconsistent use of contraception.
The most popular method of contraception chosen by Richmond residents was User Dependent Methods (UDM) such as the oral contraceptive pill and barrier methods like condoms, which at 70.8% is higher than England (62.1%). LARC excluding injections was the second most popular and used by 23.8% of residents compared with 28.1% of England residents, and injectable contraception was used by 5.3% of residents compared 9.8% of England residents (PHE, 2017).
LARC is the most effective form of contraception. LARC usage is lower than England with total prescribed LARC, excluding injections, rate with 37.3 per 1,000 compared with 46.4 in England in 2016. There were 685 attendances by Richmond residents at sexual and reproductive health services relating to LARC (excluding injections) and 1,010 LARC (excluding injections) were prescribed in primary care. However, the data do not include LARCs that have been prescribed in other services, such as termination of pregnancy (TOP) services, which may be a significant amount (PHE, 2017).
Injectable contraception is excluded from the LARC category due to reliance on users’ compliance to turn up promptly for subsequent doses every 12 weeks. In addition, emergency contraception is excluded from the LARC and user dependent methods (UDM) totals (PHE, 2017).
4.2. STI Diagnoses
In 2016, 1,309 new sexually transmitted infections (STIs) were diagnosed in residents of Richmond upon Thames, a rate of 672.2 per 100,000 residents (compared to 750 per 100,000 in England). (PHE, 2017). The overall trend for new STIs is similar to England.
4.2.2 Reinfection Rates
Reinfection rates are a marker of persistent risky sexual behaviour; between 2012 and 2016 an estimated 5.1% of women and 9.2% of men presenting with a new STI became re-infected with a new STI within 12 months. At England population level, the estimated reinfection rate was similar; 7.0% women and 9.4% of men presenting with a new STI becoming re-infected within 12 months (PHE, 2017).
4.2.3 Chlamydia
Chlamydia is one of the most common sexually transmitted infections and is frequently asymptomatic. However, untreated chlamydia can lead to complications such as longterm pelvic pain, pelvic inflammatory disease, ectopic pregnancy and infertility in women. Sexually active young people are at highest risk. The National Chlamydia Screening Programme (NCSP) aims to control chlamydia through early detection and treatment of asymptomatic infection, so reducing onward transmission and the consequences of untreated infection. The programme screens young people aged 1524 years old and treats those with detected chlamydia and their partners.
In 2016, 25.6% of the eligible population was tested. 4558 tests were carried out with 298 positives, which represents 6.5% of those tested. The chlamydia detection rate per 100,000 young people aged 15-24 years was 1,672 (compared to 1,882 per 100,000 in England) in 2016; Richmond is ranked 25th out of 33 for London (with 1 being the highest rate) and 157th out of 326 local authorities in England (PHE, 2017). The low detection rate could reflect both the success of the targeted approach of the NCSP and the relatively low infection rates in Richmond.
4.2.4 Gonorrhoea
Untreated gonorrhoea can lead to complications such as long-term pelvic pain, pelvic inflammatory disease, ectopic pregnancy and infertility in women. Prevalence is highest amongst young adults, black Caribbean people and MSM (Surveillance of antimicrobial resistance, 2017)
In 2015-16 the rate of gonorrhoea diagnoses per 100,000 was 55.5 (compared to 64.9 per 100,000 in England). The number diagnosed has risen since 2012 from 95 diagnoses to 110 in 2016, however this masks year on year increases between 2013 and 2015 when the numbers were 125, 150 and 170, and therefore the number diagnosed in 2016 is lower than in 2015.
Figure 2: Rates per 100,000 population of diagnoses of gonorrhoea by year in Richmond upon Thames compared to rates in areas of London PHE Centre (PHEC) and England: 2012-2016
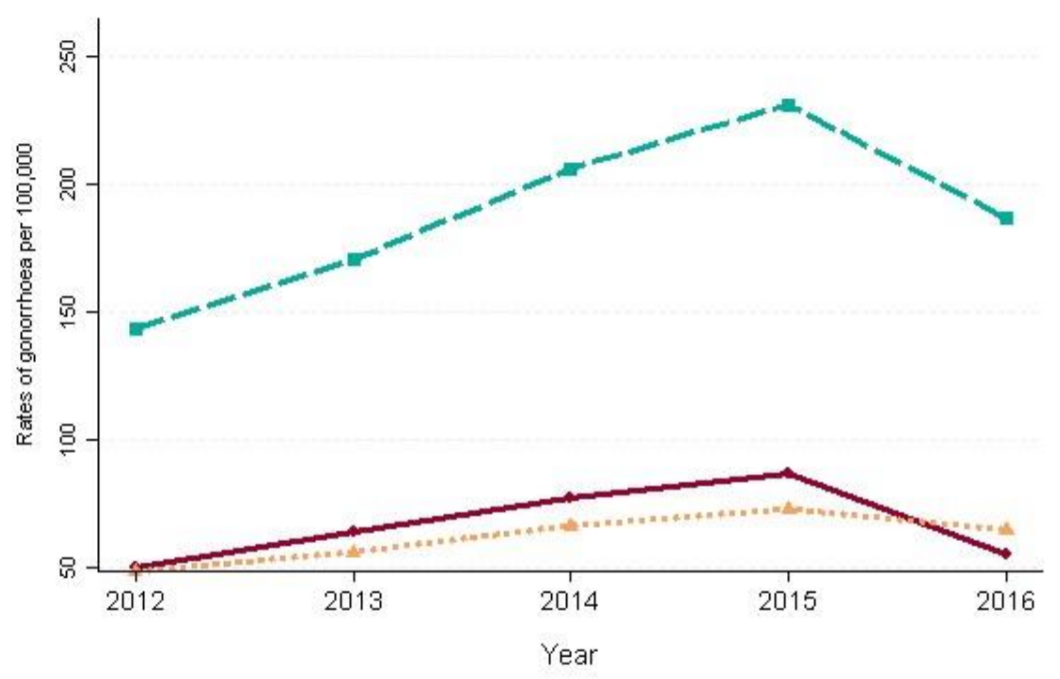
Source: Data from routine specialist and non-specialist sexual health services’ returns to GUMCAD. *Any increase in gonorrhoea diagnoses may be due to the increased use of highly sensitive Nucleic Acid Amplification Tests (NAATs) and additional screening of extragenital sites in MSM. Rates are calculated using ONS population estimates.
4.2.4.1 Gonococcal Resistance.
In 2016 the first documented global case of treatment failure (antibiotic resistance) was detected in the UK. Cases have occurred in both MSM and heterosexuals, and have been reported from across England, although more than 50% of cases were from London in 2017. As of June 2017, nationally there were a total of 81 confirmed cases. (PHE, 2017)
4.2.5 Syphilis
Syphilis is caused by bacteria and, if left untreated, it can have very serious complications, however, it is easily treated. At 14.9 per 100,000 in 2015-2016 the rate is higher than the England rate of 10.6 per 100,000. Most syphilis diagnoses are in men, especially MSM, and high rates of syphilis are associated with risky behaviour (PHE, 2017). Men who are infected with syphilis have an increased likelihood of developing HIV in the future.
4.2.6 Genital Herpes
Herpes is a long-term condition caused by the herpes simplex virus. There is no treatment for herpes, but medications can reduce the duration and frequency of herpes outbreaks.
125 residents were diagnosed with Herpes in 2016, which represents 63.7 per 100,000 higher than England 57.2 per 100,000. This is similar to 2012, when 133 residents were diagnosed.
4.2.7 Anogenital Warts
Genital warts are caused by strains of the HPV virus and can be very uncomfortable but can easily be treated.
In 2016, 265 residents were diagnosed with genital warts. This is significantly higher than England with 135.1 per 100,000 compared to 112.5 per 100,000 in 2015-2016. It is also an increase from 2012 when 230 people were diagnosed. But between 2009 and 2012 there a 14% decrease in the diagnosis rate and the overall recent trend is for Richmond to have a similar rate to England.
Figure 3: Number of cases of Anogenital warts (first episode) diagnosed in residents in Richmond 2012 – 2016
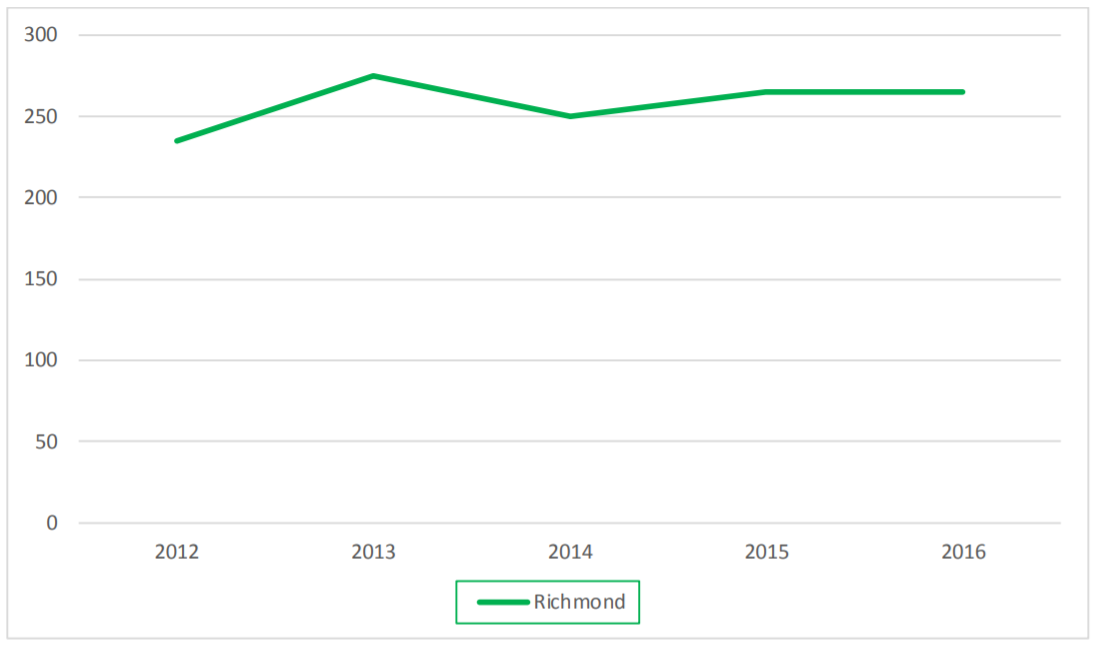
Source: Data from routine specialist and non-specialist sexual health services’ returns to the GUMCAD STI Surveillance System. Excludes chlamydia data from routine non-specialist sexual health services’ returns to the CTAD Chlamydia Surveillance system (CTAD). Rates based on the 2011 ONS population estimates.
4.2.7.1 HPV Vaccination
HPV vaccine (Gardasil) protects against four strains of HPV that can cause cancer and prevents genital warts. It is routinely offered to girls aged 12 to 13 years, and more recently to MSM, trans men and trans women who are eligible, helps to protect against genital warts and cervical cancer. In Richmond, 85% of 12 -13-year-old girls received the HPV vaccine in 2016, which is similar to London and England
The vaccination prevents at least 7 out of 10 cancers of the cervix (70%) and potentially more in the future. As it usually takes between 10 and 20 years for a cancer to develop after HPV infection the reduction in the number of cases of pre-cancerous changes in the cervix will only be seen in the longer term
4.3 HIV
HIV is a life-long condition, which currently has no cure but, with early diagnosis and treatment, people can maintain their everyday life and health. Early diagnosis and treatment can also limit onward transmission. The lifetime cost for treating one HIV infection in the UK is estimated to be almost £380,000, based on a median life expectancy of 71.5 years for MSM diagnosed at the age of 30 (Nakagawa F et al., 2015).
As a London Borough, Richmond supports the Fast-Track Cities initiative, which aims to end new HIV infections by 2030 (Mayor of London, 2018), and associated initiatives such as ‘Do It London’, which is a London-wide prevention campaign promoting HIV testing and other positive approaches to improving sexual health, launched in 2015 and funded by LAs.
Nationally, in 2017 there has been a decline in HIV diagnosis in MSM for the first time in over 30 years as well as a continued decline in black heterosexual men and women. However, rates amongst white heterosexual men and women have remained at a similar level for the last 10 years (PHE, 2017).
The HIV prevalence is 2.4 per 1,000 in 2016, the same as 2012, and Richmond is classed as a high prevalence area. NICE guidance classifies between 2 and 5 cases of diagnosed HIV per 1,000 people aged 15-59 years as high prevalence. This compares with 2.3 per 1,000 nationally.
In 2016, 346 residents were receiving HIV-related care: 275 males and 75 females. This represents a 15.3% increase from 2012 to 2016. The percentage of black people receiving HIV care is disproportionately higher than the percentage in the general population with 18.8% Black African and 1.4% Black Caribbean receiving care whereas 1.5% of the population is black. With regards to exposure, 63.6% probably acquired their infection through sex between men and 33.2% through sex between men and women.
The rate of new diagnosis is lower than England. In 2016, 13 residents aged 15 years and above were newly diagnosed, with a rate of new HIV diagnosis 8.3 per 100,000 population compared to 10.3 in England. HIV testing coverage for SHS patients is higher in Richmond than England (74.5% compared with 67.7%) (PHE, 2017).
However, in Richmond, between 2014 and 2016, over a third (35.3%) of people diagnosed with HIV were diagnosed late. Late diagnosis can result in damage to the immune system and transmission to others. The late diagnosis rate is also higher among heterosexuals (50%).
In 2016, an estimated 89,400 people were living with HIV infection in England, of whom an estimated 10,400 (11.6%) were unaware and at risk of unknowingly passing on the virus to sexual partners. If this is applied to the Richmond population, it would equate to about 45 people.
4.4 Health Inequalities
In Richmond, as in England, young heterosexual adults, black ethnic minorities and MSM experience poor sexual health disproportionately.
4.4.1 Age
4.4.1.1 Young People
Young people aged 15-24 years of age have the highest rate of new STI diagnoses with 44% of diagnoses occurring in this age group in 2016. In 2012 the rate was similar with over 40% of diagnoses occurring in this age group in Richmond. Almost two-thirds (60% or 339/559) of diagnosis occurred in this age group occurred in females.
Young people have a greater risk of being re-infected with STIs than the general population. In Richmond almost 10% (estimated 9.1%) of 15-19-year-old women and 8.9% of 15-19-year-old men presenting with a new STI at a SHS during the 5-year period from 2012 to 2016 became re-infected with an STI within 12 months. This may be because teenagers may be at increased risk of re-infection because they lack the
skills and confidence to negotiate safer sex.
4.4.1.2 Older Adults
Over the last 60 years’ sexual lifestyles in Britain have changed significantly especially amongst women. Sexual activity continues into later life, so a life course approach is needed (Mercer et al, 2013)
With more older people than in previous generations becoming newly single through divorce, separation, or the death of their partners. Many older people may have incomplete or incorrect knowledge about sexual health and therefore don’t use condoms to reduce the risk of contracting STIs when beginning new sexual relationships.
In 2016, 10% (136) of new STIs were diagnosed in Richmond residents aged between 45 and 65 years of age.
Figure 4: Proportion of new STIs by age group and gender in Richmond upon Thames: 2016
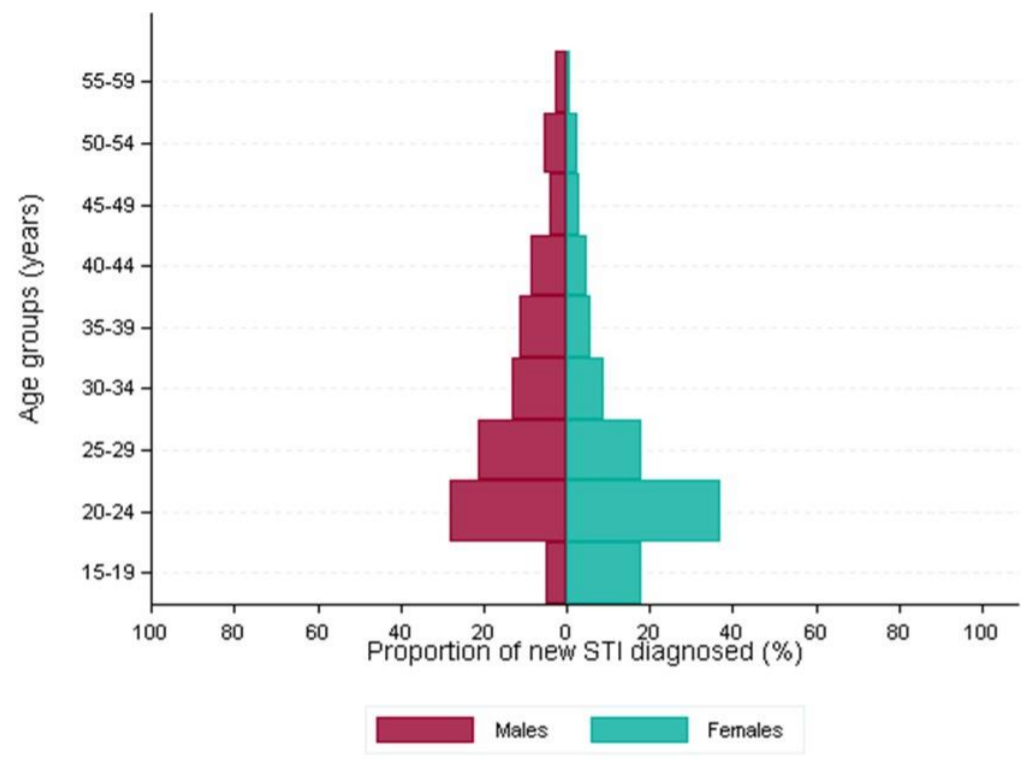
Source: Data from routine specialist and non-specialist sexual health services’ returns to the GUMCAD STI Surveillance System and routine non-specialist sexual health services’ returns to the CTAD Chlamydia Surveillance system (CTAD). *Please note that to prevent deductive disclosure the number of STI diagnoses has been rounded up to the nearest 5. From Laser Report, 2017.
4.4.2 Sexual Health Knowledge amongst Young People
Young people want more information on sexual health. In 2014 Richmond young people’s health survey showed understanding of contraception methods among secondary school pupils in Richmond was generally good but could be improved. 74% of secondary school pupils stated that the use of condoms was reliable to stop pregnancy, which is in an increase from 58% in 2012. But only 29% of pupils knew
that there is a contraception service for young people available locally.
In September 2020 state primary and secondary schools will have a statutory duty to deliver RSE (Relationships and Sex Education). Currently SRE is delivered by teachers, school nursing service, voluntary agencies and youth service.
4.4.3 Lesbian, gay, bisexual, trans gender, questioning and intersex people
In 2016, 29.4% (200 diagnoses) of new STIs in Richmond were among gay, bisexual and MSM, which is similar to 2012 (27.5% and 195 diagnoses) in 2012. There were 65 new diagnoses of gonorrhoea and 25 new diagnoses of syphilis in MSM in Richmond in 2016. This compares with 15 % of STI diagnosis were in MSM, and 65% of gonorrhoea cases and 86% of syphilis cases among men diagnosed with STIs were
in MSM England. ONS estimates suggest that 1.8% (3,000) of Richmond residents identify as Lesbian, gay or bisexual, so as group they disproportionately experience STIs.
The number of STI diagnoses in MSM has risen sharply in England over the past decade. This is possibly due to:
- Condomless sex associated with HIV seroadaptive behaviours or sexual behaviours employed by homosexual men to reduce the risk of transmitting or acquiring HIV while engaging in unprotected anal intercourse (UAI). For HIV negative men, these are serosorting (restricting any UAI to sexual partners who are also HIV-negative), and strategic positioning (restricting UAI to taking the insertive role only).
- ‘Chemsex’ (the use of drugs before or during planned sexual activity to sustain, enhance, disinhibit or facilitate the experience).
- Increased screening of MSM has improved detection of gonococcal and chlamydial infections but has had less impact in recent years as it has become more established. (PHE, 2017)
Gonorrhoea diagnosis in MSM in England decreased between 2015 and 2016, following year on year rises since 2008. This coincides with reductions in HIV diagnoses which are associated with improved HIV testing uptake at STI clinics (particularly in central London). When combined with increased STI testing uptake at STI clinics, this has potentially facilitated prompt identification and treatment of asymptomatic infection which reduces the likelihood of secondary transmission. However, gonorrhoea remains the most commonly diagnosed STI amongst MSM.
Research shows that nationally teenage lesbian or bi-sexual women are at increased risk of unintended pregnancy compared to their peers. Although there is a lower rate of pregnancy in LBWSW than the general population (around half of LBWSW are parents), there is a statistically significant higher rate of pregnancy in adolescent lesbians and bisexual women. In bisexual adolescents the rate was twice that of a heterosexual adolescent. This may be due to the higher reported rates of forced sex1 amongst LBWSW compared with the general population (Hodson, Meads and Bewley, 2017). STI infection rates are not included due to low numbers for women who have sex women (WSW).
1 Forced sex is a type of sexual abuse, defined by ChildLine as ‘being forced to have sex (intercourse), look at sexual pictures or videos, do something sexual” and it can also refer to being pressured to engage in sexual activity in return for money or drugs, often referred to as ‘transactional sex’.
4.4.3 Ethnicity
Black people, especially those of black African ethnic groups are more at risk of sexually transmitted infections, including HIV. STI diagnoses are disproportionately experienced in the black population compared to other ethnic groups; Black people make up 1.5% (3,000) of Richmond’s population but are diagnosed with 4.8% (55) of STIs. In contrast, the white population make up 88% (171,000) of the population but only 80.3% of STI infections, the Asian population make up 4% (8,000) have a similar diagnosis rate of 3.9% (45) and mixed/other make up 6% (12,000) of the population and a similar number of diagnoses (6.6 %/35) (PHE, 2017).
4.4.4 Deprivation
Nationally deprivation and socio-economic status are associated with poorer sexual health and higher teenage pregnancies (PHE, 2018, Tanton et al., 2015). However, as in 2012, there is no clear association within Richmond.
4.4.5 People with disabilities
People with a disability have the same sexual health needs as other people. However, they are much less likely to have access to information on sexual health because of attitudes towards disability and sexuality, lack of resources and lack of professionals qualified to provide the right kind of information and appropriate support. In 2018, 2,802 (2%) people aged 16-74 years consider themselves to be economically inactive due to a permanent sickness or disability (JSNA)
4.4.6 Homeless People
Homeless people are at greater risk of poor sexual health compared with the general population. This includes STIs and unplanned pregnancies and they may be vulnerable to sexual abuse; for example, if they come under pressure to exchange sex for food, shelter, drugs and money.
In 2016-17 there were 128 rough sleepers in Richmond borough (JSNA, 2018). Rough sleepers have complex needs: 96% of people living in SPEAR supported accommodation have mental health needs and 30% have a significant physical health issue. In addition, 60% have an issue with alcohol and/or substance misuse (JSNA, 2018).
4.4.7 Sex Workers
There is limited data available about sex workers. However, female sex workers are
assumed to be at increased risk of sexually transmitted infections (STIs) but there are
limited comparative data with other population groups available.
Estimates suggest 60 000 – 80 000 sex workers live in the UK and approximately 80%
are women, who work on the streets or in various indoor environments (HOC, 2016).
However, most sex workers are now thought to operate online. 9% of British men have
admitted previously paying for sex.
4.4.9 Child Sexual Exploitation
Child sexual exploitation (CSE) is a type of sexual abuse in which children are sexually exploited for money, power or status. A common feature of CSE is that the child or young person does not recognise the coercive nature of the relationship and does not see themselves as a victim of exploitation.
The complex and hidden nature of Child Sexual Exploitation means that it is very difficult to provide an accurate number of either current or former victims.
CSE/county lines2 are both a key LSCB concern in line with other outer London boroughs (PH CSE JSNA 2017 and action plan from the LSCB CSE/missing person
subgroup).
2 County lines describes how gangs from large urban areas use vulnerable adults and young people to supply drugs to suburban and rural areas. This tactic enables the gang to sell drugs in an area outside of the area they live and reduces their risk of detection. This is an issue affecting all London boroughs and its effects can be seen in many other towns and cities across England.
Child sexual exploitation (CSE) is a type of child sexual abuse. It occurs where an individual takes advantage of an imbalance of power to coerce, manipulate or deceive a child or young person under the age of 18 into sexual activity (a) in exchange for something the victim needs or w ants, and/or (b) for the financial advantage or increased status of the perpetrator or facilitator. The victim may have been sexually exploited even if the sexual activity appears consensual. Child sexual exploitation does not always involve physical contact; it can also occur through the use of technology (Department for Education,2017)
4.4.10 Risky Behaviour
The cumulative risk from multiple unhealthy behaviours is significant and these risk taking behaviours can also play a role in influencing risky sexual behaviour. Over a fifth (22%) of 15-year-olds in Richmond have 3 or more risky behaviours, including smoking, drinking, cannabis, other drugs, diet and physical health, which is the highest in London (What About YOUth? Survey 2014/15). Risky behaviour can be associated with sexting, sexual health and mental health and chemsex.
A strategic Risky Behaviour Services Review (LBRuT, 2018) was undertaken with professionals working with young people across the borough and young parents were identified as a key risk group. Although numbers are small, the need and level of vulnerability are both high.
5 Local Services
National Context
Sexual health services are commissioned at a local population level to meet the needs of the local population. These services provide information, advice and support on a range of issues, such as sexually transmitted infections (STIs), contraception, relationships and unplanned pregnancy.
Local authorities have a statutory duty to commission comprehensive open access sexual health services (including free STI testing and treatment, notification of sexual partners of infected persons and free provision of contraception) for their residents. However, some specialised services are directly commissioned by clinical commissioning groups (CCGs), and at the national level by NHS England.
Local Context
The London Borough of Richmond (LBR) commissions CLCH to provide a comprehensive open access sexual health service. The service is jointly commissioned with the London Boroughs of Merton and Wandsworth.
LBR also commissions sexual health services including Chlamydia screening and treatment, partner notification and Emergency Hormonal Contraception (EHC) via primary care. Additional preventive services are provided by the voluntary sector and through schools, school nursing and the youth service.
Sexual health services currently focus on treatment for sexual health transmitted infections, HIV and unplanned pregnancies as well as prevention. Evidence shows that increased preventive work has the potential to deliver savings not only to sexual health commissioners but to the whole system.
5.1 Integrated Sexual Health Service
In October 2017 a new service provider, CLCH, began providing an integrated hub and spoke sexual health service across Merton, Richmond and Wandsworth.
The integrated model provides screening and treatment for STIs as well as contraception. There are currently two hubs and several spokes, but a larger hub near Clapham Junction Stations will replace the smaller hubs in October 2018. Hubs provide the full range of sexual health services (levels 1-3) and spokes provide services (levels 1-2). Full details of sexual health levels can be found in appendix 1.
CLCH have provided the locally commissioned service from October 2017 using an integrated hub and spoke sexual health service across Merton, Richmond and Wandsworth. This service is open access and can be attended by non-residents just as non-residents can attend sexual health services elsewhere.
Services Attended by Residents
Between 1st October 2017 and March 31st, 2018, the sexual health service based at Kingston Hospital has the largest attendance by Richmond residents with over a third (39.4%) of residents attending. More than 13% of residents attended the service based at West Middlesex Hospital and 10.3% attended services based in Wandsworth. Compared with1st October 2016 – March 31st, 2017 shows that almost 10% of patient flow has shifted from West Middlesex Hospital to Kingston Hospital; with Kingston Hospital was still the most attended service with 28.5% of residents, 23.2% attended West Middlesex Hospital and 10.3% attended Wandsworth services. This change could be due to the changes in service provider and service locations. However, further analysis is needed to understand this.
5.2 General Practice
5.2.1 LARC
Most practices (20 out of 29) are commissioned to deliver IUD/IUS in Richmond and 17 practices out of 29 deliver Nexplanon.
5.3 Community Pharmacy
Community pharmacies are commissioned to deliver level 1 and 2 sexual health services. This includes Emergency Hormonal Contraception (EHC) for women aged 16 – 25 years of age, Chlamydia screening for 16 – 24 years of age and free condoms via the Come Correct condom distribution scheme.
5.3.1 Chlamydia Screening
As part of the National Chlamydia Screening Programme general practitioners and community pharmacists are commissioned to deliver chlamydia screening and treatment. Between 2015-2018, 371 young people aged between 16 and 24 years of age were screened for chlamydia and 73 young people were treated for chlamydia.
5.3.2 Emergency Hormonal Contraception
Between 2015-2018, EHC was prescribed on 544 occasions in community pharmacy.
5.4 Condom Distribution
The Come Correct (or CCard) scheme provides access to free condoms in a variety of locations (called Outlets) across London. Once registered, young people can collect condoms for free or get advice from any Outlet displaying the Come Correct logo. In Richmond the scheme is administered by Metro.
Between October 2017 and April 2018, 413 young people accessed the scheme in the borough with 262 young people registering for the CCard and 149 registered young people accessing condoms at venues in Richmond. Less than a quarter (59 out of 262) young people accessing the service were resident outside Richmond.
5.5 Abortion Services
Abortion services are provided by NUPAS under a South-West London contract.
More detail to follow
6 Conclusion
Overall the sexual health of the Richmond is good when compared to London and England. However, the burden of sexual ill health is disproportionate across the population; young people, black ethnic groups and MSM are more likely to suffer sexual ill health. Young people are the largest group diagnosed with a new STI and, although the teenage pregnancy rate is low, the relatively high abortion rate, with 80% of under 18 conceptions ending in abortion, indicates that a significant number of pregnancies are unplanned. Richmond young people also have the highest level of risky behaviour in London. The black population experience a significantly higher proportion of STI diagnoses compared with the proportion of the population from these ethnic groups. STI diagnosis is increasing amongst men who have sex with men.
7 Recommendations
Six priorities for action have been identified:
- To reduce the prevalence of sexually transmitted infections
- To reduce unplanned pregnancies
- To continue to reduce teenage pregnancy
- To reduce late HIV diagnosis
- To reduce risky behaviour and improve sexual health
- To take a whole systems approach to addressing priorities 1-5.
8 References
FPA. (2015) Unprotected Nation 2015: An update on the Financial and Economic Impacts of Restricted Contraceptive and Sexual Health Services. 2015.
Hodson, Meads and Bewley. (2017) Hodson, K., Meads, C. and Bewley, S. (2017) Lesbian and bisexual women’s likelihood of becoming pregnant: a systematic review and meta-analysis. BJOG: An International Journal of Obstetrics and Gynaecology, 124 (3). pp. 393-402
House of Commons (HOC), (2016) House of Commons Home Affairs Committee Prostitution Third Report of Session 2016-17
London Borough of Richmond-upon-Thames (2017) Children and Young People’s Plan 2017 to 2020
London Borough of Richmond-upon-Thames (2018) Joint Strategic Needs Assessment (JSNA)
London Borough of Richmond-upon-Thames (2018) Risky Behaviour Review
Lee, E., Clements,S., Ingham, R. and Stone, N. (2004) A matter of choice? Explaining national variation in teenage abortion and motherhood Rowntree Foundation: York
Mercer C. H. Et al (2013) Changes in sexual attitudes and lifestyles in Britain through the life course and over time: findings from the National Surveys of Sexual Attitudes and Lifestyles (Natsal) The Lancet 382(9907); 1781 – 1794
Montouchet C, Trussell J. (2013) Unintended pregnancies in England in 2010: costs to the National Health Service (NHS). Contraception. 2013;87(2):149-53.
Nakagawa F et al. Projected lifetime healthcare costs associated with HIV infection. PLOS One 10(4): e01205018, 2015.
ONS (2018) www.ons.gov.uk [accessed 19th September 2018]
Public Health England (PHE) (2017) Local Authority STI and HIV Epidemiology Report (LASER): London Borough of Richmond PHE: London
Public Health England (PHE) (2018) National Teenage Pregnancy Prevention Framework PHE: London
Richmond LSCB (2017): Richmond LSCB Annual Report 2016-17
Tanton, C., Jones, K.G., Macdowall, W., Clifton, S., Mitchell, K.R., Datta, J., Lewis, R.,
Field, N., Sonnenberg, P., Stevens, A., Wellings, K., Johnson, A.M. & Mercer, C.H. (2015) Patterns and trends in sources of information about sex among young people in Britain: evidence from three National Surveys of Sexual Attitudes and Lifestyles. BMJ Open [online]. 5(3). [Accessed 4th June 2018]
WAY Survey (2014) Available from: https://digital.nhs.uk/data andinformation/publications/statistical/health-and-wellbeing-of-15-year-olds-inengland/main-findings— 2014
WHO (2006) Defining sexual health: Report of a technical consultation on sexual health, 28-31 January 2002, Geneva, https://www.who.int/reproductivehealth/publications/sexual_health/defining_sexual_he
alth.pdf [accessed 3rd September 2018]
Appendix 1
Sexual Health Service Definition of Levels
Level 1
- Sexual history-taking and risk assessment: Including assessment of need for emergency CONTRACEPTION and Human Immunodeficiency Virus (HIV) postexposure prophylaxis following sexual exposure (PEPSE)
- Signposting to appropriate Sexual Health Services
- Chlamydia screening: Opportunistic screening for genital chlamydia in asymptomatic males and females under the age of 25
- Asymptomatic Sexually Transmitted Infection screening and treatment of asymptomatic infections (except treatment for syphilis) in men (excluding men who have sex with men) and women
- Partner notification of Sexually Transmitted Infections or onward referral for partner notification
- Human Immunodeficiency Virus testing: Including appropriate pre-test discussion and giving results
- Point of care Human Immunodeficiency Virus testing: Rapid result Human Immunodeficiency Virus testing using a validated test (with confirmation of positive results or referral for confirmation)
- Screening and vaccination for Hepatitis B: Appropriate screening and vaccination for Hepatitis B in at-risk groups
- Sexual health promotion: Provision of verbal and written sexual health promotion information
- Condom distribution: Provision of condoms for safer sex
- Psychosexual problems: Assessment and referral for psychosexual problems
Level 2
Level 2 Sexual Health Services incorporate Sexual Health Services provided by a Level 1
Sexual Health Service plus:
- Intrauterine Device/System (IUD/IUS) insertion and removal (including emergency IUD)
- CONTRACEPTION implant insertion and removal
- Counselling and referral for vasectomy
- Sexually Transmitted Infection (STI) testing and treatment of symptomatic but uncomplicated infections in men (except men who have sex with men) and women excluding: men with dysuria and/or genital discharge, symptoms at extra-genital sites, e.g. rectal or pharyngeal, pregnant women, genital ulceration other than uncomplicated genital herpes.
Commissioned Level 2 Sexual Health Services include:
- Enhanced General Practices
- Sexual and Reproductive Health Services
- Integrated services (joint Genitourinary Medicine and Sexual and Reproductive Health
Services) - Young people clinics such as Brook
- Other NHS commissioned Sexual Health Services Level 3
Level 3
Level 3 Genitourinary Medicine Services provide Sexually Transmitted Infection (STI) management and include SERVICES provided by Level 1 Sexual Health Services and Level 2 Sexual Health Services plus:
- Sexually Transmitted Infection testing and treatment of men who have sex with men
- Sexually Transmitted Infection testing and treatment of men with dysuria and genital discharge
- Testing and treatment of Sexually Transmitted Infections at extra-genital sites
- Sexually Transmitted Infections with complications, with or without symptoms
- Sexually Transmitted Infections in pregnant women
- Recurrent or recalcitrant Sexually Transmitted Infections and related conditions
- Management of syphilis at all stages of infection and blood borne viruses
- Tropical Sexually Transmitted Infections
- Specialist Sexually Transmitted Infection (HIV) treatment and care
- Provision and follow up of Sexually Transmitted Infection post exposure prophylaxis
(PEP), both sexual and occupational - Sexually Transmitted Infection service co-ordination across a network including:
- Clinical leadership of Sexually Transmitted Infection management
- Co-ordination of clinical governance
- Co-ordination of Sexually Transmitted Infection training
- Co-ordination of partner notification
Glossary
BME Black and minority ethnic
CCG Clinical Commissioning Group
DoH Department of Health
EINA Equality Impact Needs Assessment
EHC Emergency hormonal contraception
GPs General Practitioners
HIV Human immunodeficiency virus
LARC Long acting reversible contraception
LGBTQI Lesbian, gay, bisexual, transgender, questioning and intersex
LSHTP London Sexual Health Transformation Programme
MSM Men who have sex with men
NHS National Health Service
NHSE National Health Service England
NICE National Institute for Health and Care Excellence
PHE Public Health England
PrEP Pre-Exposure Prophylactic
RSE Relationships and sex education (the new name for SRE)
SRE Sex and relationship education
STIs Sexually Transmitted Infections
UDM User dependent methods
WHO World Health Organisation
WSW Women who have sex with women
Document Information
Published: 2018
For Review: 2022
Public Health Topic Lead: Hannah Gill, Public Health Lead
